Jaundice in Newborns & Bilirubin Levels
Question
Dr. Greene, my 6-week old was diagnosed with breastfed jaundice when her bilirubin was taken at one week old. I am supposed to stop breastfeeding her for 24 hours (and give her formula) and am finding her resisting the bottle. Will the jaundice eventually go away and could there be any harm in not giving her the recommended 24-hour break from breastfeeding?
Cambridge, Massachusetts
Dr. Greene's Answer
This week, while I was putting up lights to decorate for the holidays, I bruised my arm. I can remember, as a young child, watching bruises transform through a series of colors before they eventually disappeared.
What Causes Jaundice
Hemoglobin, the red pigment in red blood cells, must undergo a succession of changes before the body can dispose of it. Specific enzymes from our great processing center, the liver, carry out each step. Bilirubin, the yellow pigment responsible for jaundice, is a normal component in the breakdown of hemoglobin. Adults often turn yellow when they have hepatitis because their livers aren’t able to process the bilirubin.
Every day, about 1% of our red blood cells expire, to be replaced by fresh, young ones ready to carry oxygen to supply the body. Our lifeblood is new every 4 months.
A low level of bilirubin (about 1 mg/dL) circulates throughout our bodies as part of this process. This concentration is too faint to be visible or cause any harm.
Even before babies are born, this renewing of the blood is taking place. The placenta carries away the bilirubin as it is formed to the mother’s liver to be processed. After babies are born, they enter a transition period as their livers begin to assume this responsibility. Often, their immature livers can’t quite keep up.
The presence of enough bilirubin for the yellow pigment to be visible is called jaundice. Jaundice occurs in about 60% of healthy term infants and 80% of those born prematurely (mainly due to the immaturity of their livers before 37 weeks). If the bilirubin concentration rises to about 5 mg/dL, the face takes on a yellow appearance. If the level reaches about 15 mg/dL, the yellow tint is visible from the head down to the midabdomen. At a level of 20 mg/dL, even the soles of the feet are yellow (note: these are approximations, and a blood test is required to know the true bilirubin level).
Bilirubin is found throughout the body, not just in the skin. Under certain conditions, high concentrations of bilirubin are toxic to babies’ brains. This is very rare when the concentration is under 25 mg/dL, but at higher concentrations, an increased risk for permanent hearing loss, mental retardation, spastic quadriplegia, or even death exists. This is called kernicterus, and is preventable by measuring bilirubin levels and initiating treatment when the levels are high.
Treatment is dependent on the level of bilirubin and the calculated risk of the rate of it increasing. Treatment ranges from watchful waiting (along with rechecks of the bilirubin levels along the way), phototherapy (at home or in the hospital) and for very high levels of bilirubin treatment may be a procedure called exchange transfusion- which is the definitive way to remove bilirubin from a newborn’s blood.
Causes of Rising Levels of Bilirubin
Anything that increases the number of expiring red blood cells soon after birth makes jaundice more likely. This might include the pounding babies take during difficult births (sometimes they look like little prizefighters) or the scalp hematomas caused by vacuum-assisted deliveries (one of my children looked like the ultimate conehead!). Sometimes extra red blood cells applying for social security are the result of a blood-type incompatibility, delayed cord clamping, a congenital anemia, or an infection.
Anything that makes it tougher for the immature liver to process the bilirubin can also lead to jaundice, including prematurity, lack of oxygen, poor feeding, thyroid deficiency, a genetic enzyme deficiency, or a liver otherwise occupied with dealing with an infection.
Physiologic Jaundice
The most common type of jaundice is called physiologic jaundice, the normal increased bilirubin in babies whose livers can’t quite keep up with a slightly increased load of red blood cells. This usually becomes visible on day 2 or 3 and peaks somewhere between days 2 and 4 as the liver gains control of the situation. The bilirubin levels usually fall substantially by day 7. Sometimes, they reach a level at which treatment is needed (>15 mg/dL before 48 hours old, >18 mg/dL before 72 hours old, > 20 mg/dL anytime–in otherwise healthy term babies). Stopping nursing is not recommended for physiologic jaundice, although supplementing feeds with pumped breast milk or formula may be helpful.
Breast-feeding Jaundice
There are two types of jaundice that are related to breast-feeding. They are called breast-feeding jaundice and breast milk jaundice. Breast-feeding jaundice is common and is a jaundice that may occur in the first week of life in breast-fed infants and mostly goes away on its own as the baby increases their feeding and pooping. The cause is thought to be due to decreased milk intake leading to dehydration or low caloric intake. The incidence of breast-feeding jaundice may be reduced by increasing the frequency of feeding and refraining from using water to replace breast milk.
Breast Milk Jaundice
Breast milk jaundice is another type of jaundice that may be seen in up to 30% of predominantly breastfed babies. However, less than 2% of these babies ever have bilirubin levels reaching threshold for phototherapy treatment. This jaundice is often not visible until the baby is a week old and then reaches its peak during the second or third week and resolves by 12 weeks of age. The exact mechanism by which breast milk causes jaundice is uncertain. Breast milk jaundice may be caused by enzymes in mom’s milk that allow bilirubin to be reabsorbed into the blood from the intestines or by fatty acids in mom’s milk that the baby processes as a priority over processing the bilirubin. Or there may be an as yet unidentified mechanism.
Whichever the cause, if the mother continues to nurse her baby, the jaundice will decrease and disappear on its own, but this may take up to 12 weeks. If the mother stops nursing for 1 or 2 days, substituting formula, the bilirubin levels will drop rapidly. They will not rise again when the nursing is resumed.
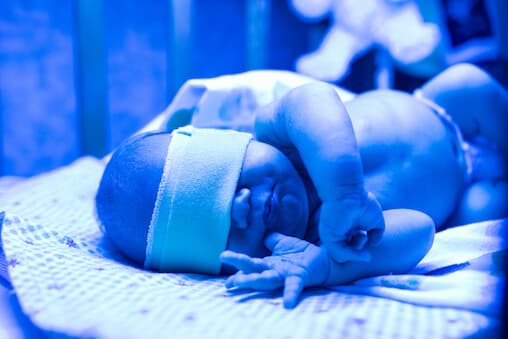
Permanent damage or ill effects from breast milk jaundice is extremely rare. Phototherapy (lights used to lower bilirubin) may be used if the level of bilirubin reaches the threshold as set by the American Academy of Pediatrics (AAP). In breast milk jaundice, stopping breast milk for 1 to 2 days can help the bilirubin level drop rapidly. However, pediatricians and neonatologists generally agree that most babies who are well enough to feed may continue to feed on breast milk. This is true even when the bilirubin level is high enough to require phototherapy.
Even as I’m writing this article, my body is silently at work healing the bruise on my arm. As surely as that bruise will be gone by the new year, if your daughter has breast-feeding jaundice, she too will soon take care of her “pigment problem” herself whether or not you take a break from nursing.
Resources and References
Bhutani V, Committee on Fetus and Newborn. Phototherapy to prevent severe neonatal hyperbilirubinemia in the newborn infant 35 or more weeks of gestation. Pediatrics. 2011; 128(4):e1046-e1052.
Maisels MJ, Clune S, Coleman K, Gendelman B, Kendall A, McManus S, Smyth M. The natural history of jaundice in predominantly breastfed infants. Pediatrics. 2014;134(2):e340-5.
Muchowski KE. Evaluation and treatment of neonatal hyperbilirubinemia. Am Fam Physician. 2014; 89(11):873-8.
Reddy DK, Pandey S. Kernicterus. [Updated 2022 Aug 28]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2023 Jan.
Subcommittee on Hyperbilirubinemia. Management of hyperbilirubinemia in the newborn infant 35 or more weeks of gestation. Pediatrics. 2004:114(1):297-316.
Seyedi R, Mirghafourvand M, et al. The effect of the use of oxytocin in labor on neonatal jaundice: A systematic review and meta-analysis. Int J Pediatr. 2017;5(12):6541-53.


