Concussion: A-to-Z Guide from Diagnosis to Treatment to Prevention
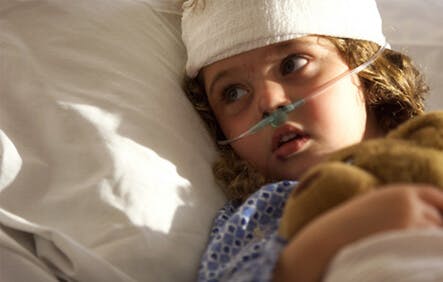
Children’s energetic exploration of life often results in head bonks. Fortunately, most of them are not serious. Nevertheless, when we hear the awful thud of a child’s head, our breath catches for a moment…
What is concussion?
A brief, temporary loss of consciousness following a blow to the head is called a concussion. It is possible to have a mild concussion without losing consciousness completely. Any brief alteration in consciousness, vision, and balance following a head injury could be a mild concussion.
Who gets concussion?
Is toddlerhood a contact sport?
Almost every child experiences minor head injuries. They occur throughout childhood and adolescence. They are most common in infants and toddlers and then later when children engage in contact sports.
What are the symptoms of concussion?
The classic symptom of a concussion is a brief loss of consciousness. A mild concussion might only cause brief confusion or momentary amnesia. It can be normal to have a headache, feel sleepy, or vomit once or twice afterwards.
In a baby or toddler, a prompt cry after a head injury is reassuring. The following is a list of signals that tell you that you need to talk with your pediatrician, either initially, or again if they develop after the first conversation:
If your child is (or has):
- Under 6 months of age
- Unconscious, even briefly
- Crying for longer than 10 minutes
- Vomiting repeatedly
- Bleeding or clear liquid from the ears or nose
- Rapid swelling just above the ear
- Unable to walk or talk normally
- Unequal pupil size
- Severe, worsening headache (or irritability before a child can talk)
- Neck pain
- Seizures
- Skull indentation or large bump
- Great force of injury (car accident, long fall, baseball bat, etc.)
- Changes in behaviour, such as being sleepy and difficult to arouse>
If any of these symptoms or situations is present, call your physician right away. Your child may be fine but you should be in touch with an expert. If your child is unable to get up by himself immediately after the head injury, there may also be a neck injury. It might be best not to move him. Call 911 and wait for emergency help to arrive.
Is concussion contagious?
Concussions and head injuries are not contagious, although the risk-taking behavior that leads to them can be.
How long does concussion last?
The loss of consciousness from a concussion may last only a few seconds, but it can last considerably longer. If it lasts a few minutes or longer, the child will likely need to be hospitalized for observation or treatment.
New symptoms can develop after a head injury during the next 24 to 48 hours, especially if there is some internal bleeding.
How is concussion diagnosed?
The nature and extent of a head injury is first assessed based on the story and on the physical exam. If there is any concern that a serious injury may be present, additional studies, such as a head CT, may be needed.
How is concussion treated?
For most concussions, observation and rest is all the treatment that is needed. During the first night afterward, you’ll want to try to awaken your child once or twice to be sure that he awakens normally.
Some children need definitive treatment at a hospital or even in a pediatric ICU for severe head injuries.
With any concussion, the risk is much higher from a second concussion soon after the first one (called the second impact syndrome) because the healing brain is not able to regulate blood flow as well.
According to the AAP Clinical Report on Sport-Related Concussion in Children and Adolescents, all children who have suffered a concussion must proceed sequentially through the following steps. A child must pass 24 hours in each step of the rehabilitation process and wait a minimum of 5 days to return to competition-level sports participation:
- No activity — Complete physical and cognitive rest
- Light aerobic activity — Walking, swimming, stationary cycling at 70% maximum heart rate; no resistance exercises
- Sport-specific exercise — Specific sport-related drills but no head impact
- Noncontact training drills — More complex drills, may start light resistance training
- Full-contact practice — After medical clearance, participate in normal training
- Return to play — Normal game play
Repeated concussions increase the risks of acute or ongoing problems. Thus, physicians generally recommend avoiding contact sports for at least two weeks after a second mild concussion (confusion without loss of consciousness), for a month after a second moderate concussion (confusion and brief amnesia), and for the season after a second severe concussion (complete loss of consciousness).
How can concussion be prevented?
Helmets for using a bicycle, scooter, or roller-blades, and helmets for contact sports can help prevent many serious head injuries. Make sure your child is properly equipped for his activities.
Stair gates for infants and toddlers and car seats or seat belts for everyone in the car are also important safety equipment.
Rock-a-Bye Baby, the lullaby about a baby toppling from a poorly placed cradle, warns parents of a real danger. Falls from open windows, rooftops, balconies, play structures, and other heights injure more children than any other cause.
Summertime is the greatest danger period, with more open windows and more outdoor play. Children love to climb, so furniture is best kept back from windowsills and balcony railings. Window guards and window stops can let fresh air in but keep a child from falling out. Don’t rely on ordinary window screens to keep your children safe. In addition, placing shrubbery or something soft under danger areas can lessen the injury if a child does fall.
Related concepts:
Head injury


